
Location
-
When To See an OBGYN
posted: Mar. 01, 2024.
Category: OBGYN Care
-
What Does an OBGYN Do?
posted: Feb. 13, 2024.
Category: OBGYN Care
-
The Importance of Regular Check-ups: Exploring the Benefits of OBGYN Visits
posted: Nov. 07, 2023.
Category: Women's Healthcare
-
Understanding the Role of an OBGYN: What They Do and Why It Matters
posted: Nov. 01, 2023.
Category: Women's Healthcare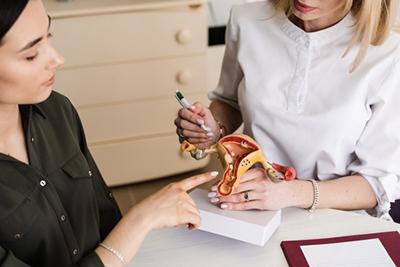
-
Benefits of Having an OBGYN
posted: Sep. 12, 2023.
Category: OBGYN Care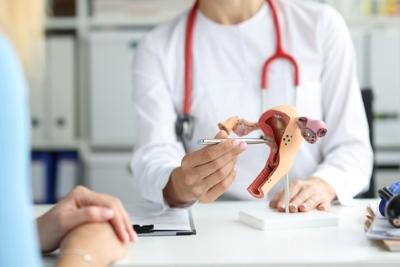
-
When To Visit an OBGYN
posted: Aug. 01, 2023.
Category: Women's Healthcare
-
When Should You See an OBGYN?
posted: Jun. 22, 2023.

