
Location
-
The Benefits of Regular Gynecological Exams
posted: Feb. 09, 2023.
Category: OBGYN, OBGYN Care, Women's Healthcare
-
Navigating the Different Birth Control Options
posted: Jan. 26, 2023.
Category: OBGYN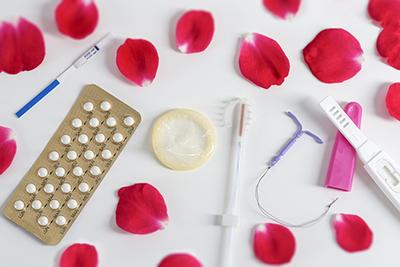
-
The Importance of Regular Gynecological Exams
posted: Jan. 12, 2023.
Category: OBGYN, OBGYN Care, Women's Healthcare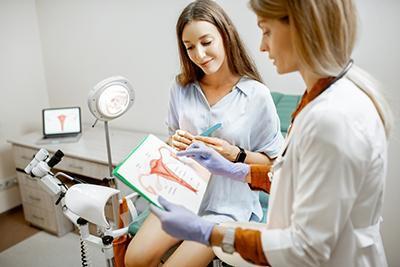
-
The Importance of Regular Gynecological Checkups for Women’s Health
posted: Dec. 29, 2022.
Category: OBGYN, OBGYN Care, Women's Healthcare
-
Contraceptive Management
posted: Dec. 12, 2022.
Category: OBGYN
-
Management of Abnormal Pap Smears
posted: Nov. 23, 2022.
Category: OBGYN, OBGYN Care, Women's Healthcare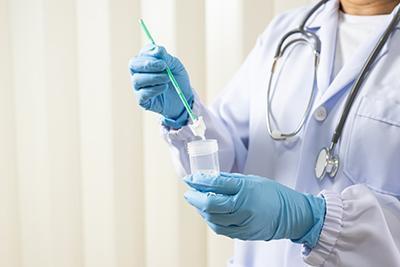
-
What Causes Pelvic Pain?
posted: Nov. 10, 2022.
Category: OBGYN, OBGYN Care, Women's Healthcare
